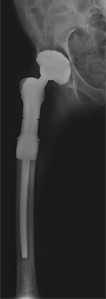
What is Proximal Femoral Resection and Reconstruction?
Benign or malignant tumors can develop in or spread to the upper (proximal) part of the femoral bone (thigh bone) causing progressive bone tissue destruction. This can be associated with pain and loss of hip function and mobility. Proximal femoral resection is a procedure to remove the diseased proximal femur which can then be reconstructed with an artificial prosthesis to restore hip function.
Tumors that usually develop in the proximal femur include primary sarcomas or metastatic carcinomas. These conditions may be treated by radiation, but if there is extensive tissue involvement and a risk of fracture, surgery is indicated. Surgery initially involved amputation of the limb and part of the hip but with advances in surgical technique and bioengineering, limb salvage is possible.
Modern prostheses come with components of different shapes and sizes. Some prosthetic implants can even expand which is necessary for patients who are skeletally immature.
Diagnosis
To diagnose your condition, your symptoms and medical history are reviewed and a history and physical examination is performed. Diagnostic tests that may be ordered include X-rays, a bone scan, MRI, or CT scan, and an angiography to evaluate neighboring blood vessels. In certain cases, a biopsy of the lesion may be needed to make a clear diagnosis. If the tumor is found to be a metastatic lesion, tests are performed to locate the primary tumor.
Indications
Your doctor will recommend proximal femoral resection and reconstruction after considering a number of factors including the extent of the tumor, its location, its radiographic features, the underlying diagnosis, your level of pain and expected survival.
Surgery is recommended if the tumor in the proximal femur is large, causing extensive bone destruction, does not respond to radiation or chemotherapy, has failed previous surgery, or is the only metastatic lesion that is present.
Preparation for the procedure
Diagnostic studies help determine the extent of bone and soft tissue resection necessary, whether a fracture is present, the proximity of the tumor to vital nerves and vessels, and the dimensions of the prosthesis required.
Some tumors are highly vascular and carry a risk of increased bleeding during surgery. Preoperative embolization (blocking off the supplying blood vessels) may be considered in such cases. In other cases, radiation may be recommended prior to surgery.
The tumor can rarely extend into the hip joint, the capsular structures, or the acetabulum (hip socket). This may happen if a fracture is present.
Certain tumors of the proximal femur if not extensive may be treated by an intramedullary nailing procedure with proximal screw fixation and supplemental cement.
Procedure for Proximal Femoral Resection and Reconstruction
This is a major procedure which is carried out under general anesthesia. You will lie on your side for the procedure. A long incision is made over the side of the buttock and upper leg. This helps expose the proximal femur, gluteal area, and superficial femoral artery. The gluteal muscles are detached. The femoral arteries and the sciatic nerve are identified and protected. The hip abductor muscles attached to the greater trochanter are identified and retracted. The capsule of the hip joint is opened with an incision and separated from the femoral neck. The femur is dislocated with care to avoid fracture of the femoral neck. The hip socket or acetabulum is inspected.
Femoral osteotomy is performed with an oscillating saw at the location determined with preoperative imaging. Care is taken to avoid injury to the soft tissues. The remaining femur is then retracted and the psoas and adductor muscles are identified, dissected, clamped, and tagged. After resection of the proximal femur, your surgeon will measure the size of the femoral head, the diameter of the medullary canal, and the length of the femur.
A trial prosthetic femoral head is then tested. The medullary canal is reamed in order to fit the stem of the prosthesis. The head, neck, and body of the prosthesis are assembled and matched with the resected proximal femur. It is then fitted in place. The joint capsule is pulled over the femoral head component. Range of motion of the hip is then tested. If satisfactory, the final prosthesis is then precisely oriented and cemented into the medullary canal. Leg length is evaluated and the important nerves and blood vessels are assessed. Care is taken to restore muscle coverage over the prosthesis and to ensure the stability of the hip joint. This helps improve function and reduces the likelihood of infection around the prosthesis.
The hip capsule is then sutured close around the neck of the prosthesis and helps holds the prosthetic head in articulation. The external rotator muscles and psoas muscles are sutured to the repaired capsule to reinforce it. The prosthesis also has components that allow additional bone and soft tissue fixation.
The retracted abductors muscles are then attached to the prosthesis. If a section of bone was separated from the greater trochanter with the abductors attached then this section of bone with its attachments is fixed to the prosthesis. Joint stability is then checked. Surgical drains are placed and the wound is closed.
Postoperative Care
Following surgery, you will be placed in a suspensory system with the operated hip elevated and abducted to 20 degrees. This is continued for 5 days and helps minimize postoperative swelling and prevent dislocation. You will then be placed in a customized hip abduction brace. You will be instructed on postoperative exercises which will begin the day after surgery. The suction drains will remain in place for 3-5 days and you will continue to be on antibiotics during this time. You will have weight-bearing restrictions for at least 3-4 weeks following surgery and should wear the brace while moving around.
Risk and Complications
Risks associated with proximal femoral resection and reconstruction include
- Joint instability and dislocation
- Infection
- Nerve and vessel injury
Femoral resection and reconstruction has good functional outcomes and is also recommended for non-tumor related conditions such as revision hip replacement surgery and persistent joint infection.

